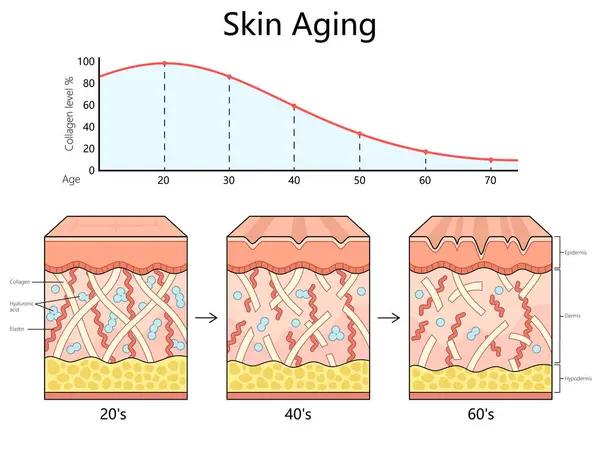
Skin elasticity is a critical factor in the field of plastic surgery, influencing both the planning and outcomes of various procedures. Assessing skin elasticity in plastic surgery clinics is essential because it provides valuable information about the patient’s skin health, age-related changes, and potential response to surgical interventions. This evaluation helps surgeons tailor treatments more effectively, ensuring better results and minimizing complications.
The skin’s ability to stretch and return to its original shape reflects its underlying collagen and elastin content. These proteins are responsible for maintaining firmness and resilience. As people age or experience environmental damage such as sun exposure or smoking, their skin loses elasticity. Reduced elasticity can affect how well the skin adapts after procedures like facelifts, tummy tucks, or breast augmentations. Without proper assessment of this property, patients might face issues such as sagging, uneven texture, or prolonged recovery times.
In clinical practice, checking for skin elasticity involves both visual examination and physical tests where the surgeon gently pinches or stretches the skin to observe its recoil speed. Advanced devices may also be used to measure biomechanical properties learn more precisely. These methods provide quantitative data that guide decision-making regarding incision placement, tension management during closure, and the choice between surgical versus non-surgical options.
Understanding a patient’s individual skin characteristics allows surgeons to set realistic expectations by explaining possible limitations based on tissue quality. For example, someone with significantly diminished elasticity might benefit from additional treatments like laser therapy or radiofrequency before undergoing surgery to improve overall outcomes. Conversely, patients with good elastic properties often experience smoother healing processes with less scarring.
Moreover, regular checks of skin elasticity contribute to personalized care plans that enhance safety standards within plastic surgery clinics. By anticipating challenges related to poor tissue compliance early on in consultations, practitioners can avoid overextending compromised areas that might lead to wound dehiscence or unsatisfactory aesthetic results.
Ultimately, integrating routine assessments of skin elasticity into preoperative evaluations fosters improved communication between surgeon and patient while optimizing procedural success rates. This approach underscores a commitment not only to cosmetic enhancement but also to preserving long-term tissue integrity through informed surgical strategies tailored specifically for each individual’s unique dermatologic profile.
In summary, monitoring skin elasticity is indispensable in modern plastic surgery settings because it directly impacts treatment customization and postoperative satisfaction levels by providing insights into tissue behavior crucial for effective intervention planning and execution.